
Diabetes dictionary (glossary)
Blood glucose (BG) or blood sugar level: The amount of glucose (sugar) found in the blood. Either term can be used. In Canada, blood sugar levels are measured as mmol/L.
Blood glucose monitor (or glucometer): A medical device used to check blood glucose level. A drop of blood is placed on a test strip, which is inserted into a hand-held meter. Students with diabetes are encouraged to keep their meter with them at all times.
Carbohydrate (CHO or carb): Sugars, fibres or starches found in many processed and unprocessed foods. Examples of carb-containing foods include breads, cereals, beans, pasta, fruits, milk, potatoes, and more. Carbohydrates provide the body with glucose (sugar), and are its main source of energy. Eating carbs raises blood sugar level, but some carbs work more quickly than others (see Fast-acting sugar).
Celiac disease: A medical condition that causes an immune reaction to eating gluten, which is a protein found in wheat, rye and barley. It causes damage to the intestines and symptoms like stomach pain, bloating, and diarrhea. People with celiac disease must follow a gluten-free diet. Up to 10% of people with type 1 diabetes also have celiac disease.
Continuous Glucose Monitor (CGM, sensor): A device that provides a blood glucose reading every 5 minutes through a small sensor inserted under the skin.
Correction factor (CF) (or insulin sensitivity factor (ISF)): Unique to each person, it is the amount that 1 unit of fast-acting insulin will lower a person’s blood sugar. People with diabetes use correction factors to adjust insulin doses for the blood sugar level at the time of the dose.
Diabetes Kit (also called Hypokit, Safe kit, Emergency Kit): A sturdy container, such as a plastic box, with all the supplies needed to treat high or low blood sugar (especially low) and any other equipment that a student with diabetes needs. The specific contents of a student’s kit should be described in the Individual Care Plan.
Diabetic ketoacidosis (DKA): A serious complication of diabetes caused by not having enough insulin. Symptoms include abdominal pain, nausea, vomiting, high blood sugar and ketones (which cause fruity-smelling breath). Without treatment, DKA can be life threatening.
Fast-acting sugar: A source of carbohydrate (sugar) that the body can quickly absorb, raising blood sugar levels. Examples include juice and candy. Fast-acting sugars are used to treat mild to moderate low blood sugar levels (hypoglycemia). A student with diabetes should always have a source of fast-acting sugar close by.
Glucagon: A hormone that raises blood sugar. An injectable form of glucagon is used to treat severe low blood sugar levels (hypoglycemia) when a person is not able to take fast-acting sugar by mouth (in the case of unconsciousness, for example).
Glucometer (or blood glucose meter): A medical device that is used to check blood sugar (glucose) level. A drop of blood is placed on a test strip, which is inserted into a hand-held meter. Students with diabetes are encouraged to keep their meter with them at all times.
Glucose (sugar): Fuel that the body needs to produce energy. Glucose comes from carbohydrate-containing foods such as breads, cereals, fruit and milk.
Hyperglycemia: Also called high blood sugar (glucose), hyperglycemia is when a person’s blood sugar level is higher than the target range. Sometimes this condition needs an urgent response.
Hypoglycemia (mild or moderate): Also called low blood sugar/glucose, mild or moderate hypoglycemia is an urgent situation and a potential emergency. It occurs when a person’s blood sugar level drops below the target range. Hypoglycemia must be treated immediately with fast-acting sugar. Blood glucose must be monitored until the level is stable and returns to the target range. Hypoglycemia can be caused by: too much insulin, too little food, or too much physical activity without extra food.
Hypoglycemia (severe): An urgent and life-threatening emergency. Someone with severe low blood sugar needs another person’s help immediately. Symptoms include confusion, fainting, seizure, and difficulty speaking.
Individual Care Plan (ICP): A document with all details of the student’s condition and specific care directions for the school.
Insulin: A hormone, released by the pancreas, which converts glucose (sugar) into energy. Without insulin, glucose builds up in the blood instead of being used for energy. People with type 1 diabetes do not produce their own insulin, so must administer it by syringe, pen or pump.
Insulin pen: A device used to inject insulin.

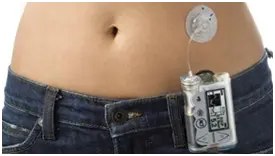
Insulin pump: A device that administers insulin continuously through a smalltube inserted under the skin. The pump is also used to give extra insulin with meals or to correct high blood sugar levels.
Ketones: Chemicals produced by the body when there is not enough insulin. Ketones can make a person with diabetes feel sick and can lead to serious illness (see Diabetic ketoacidosis, DKA). Ketones can be checked using a meter (with a drop of blood) or with urine test strips. A student’s care plan will have details on when to check for ketones.
Lancets: Small needles that are inserted into a lancing device and used to prick the skin (usually a finger) for a blood sugar check. Lancets are to be used only once. Used lancets must be safely disposed of in a sharps container.
Sharps: Used syringes, insulin pen needles, or lancets must be disposed of carefully in appropriate containers.
Target range: Desirable blood sugar (glucose) levels, which are personalized for the student. Target ranges are based on Diabetes Canada's Clinical Practice Guidelines.
Test strip: A small disposable strip used to measure blood sugar (glucose) levels. The strip is inserted in a blood glucose meter, then a lancet is used to get a small drop of blood from a finger. Each test strip can be used only once.
Type 1 diabetes: A medical condition where the pancreas no longer produces insulin, the hormone that regulates blood glucose. Without insulin, blood glucose levels build up in the blood, leading to increased thirst and urination, and decreased energy. Type 1 diabetes is an auto-immune disease, and it used to be called juvenile diabetes.
Type 2 diabetes: A medical condition where the body does not respond well to insulin, and the pancreas cannot produce enough insulin to compensate. Type 2 diabetes is more common in adults than in children and youth, and is different from type 1 diabetes.
Source : Diabetes@school. diabetesatschool.ca © Canadian Paediatric Society
Last updated: